A novel approach to the MILD procedure.
- CASE example:
- 86 y/o M veteran with CLBP and pain in legs when he walks. He and his wife estimate 100 feet without sitting/resting.
- Severe dementia, cannot recall his wife’s name, who accompanies him.
- He rides his bicycle 20 miles daily without leg pain.
His MRI:
L2-3:
4mm right paracentral disc protrusion
Bilateral moderate hypertrophy of ligamentum flavum
No evidence of central canal narrowing
Bilateral mild to moderate neural foraminal narrowing
L3-4:
4mm right paracentral disc protrusion
Bilateral moderate to severe hypertrophy of ligamentum flavum
Mild central canal narrowing with 7mm AP diameter of the canal
Bilateral mild to moderate neural foraminal narrowing
L4-5:
7mm uncovered disc due to anterolisthesis of L4 on L5
Bilateral severe hypertrophy of the ligamentum flavum
Severe central canal narrowing with 5mm AP diameter of the canal
Bilateral mild to moderate neural foramina narrowing
L5-S1:
6-7mm uncovered due to retrolisthesis of L5 on S1
No evidence of central canal narrowing
- Literature:
- Lumbar Spinal Stenosis a common undertreated cause of back pain and neurogenic claudication (Katz JN 2008, Kalichman, L 2009)
- Previously:
- ESIs or Open Laminectomy +/- fusion
Outpatient procedure / Percutaneous technique.
Relatively safe – most invasive part of procedure is placement of epidurogram.
Improves patient’s symptoms ~75% of the time (Basu S 2010)
-compared to open decompression in which 64% of patients improve (Turner JA 1992)
High levels of patient satisfaction in multiple studies.
Decreases health care resource utilization (Wang, J. Bowden, K. 2013)
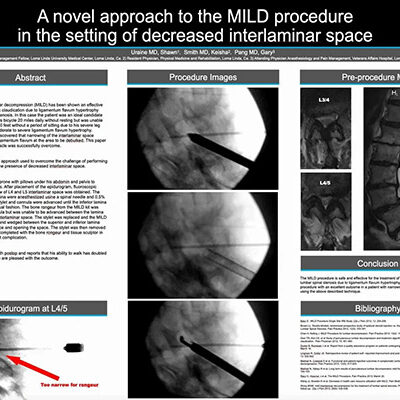
Procedure successfully decompressed his stenosis, epidurogram widened, procedure was a success.
- Patient’s wife sent a card, thanking us for what we did and how the procedure made their vacation a success.
- On follow up he and his wife report the distance he can walk has at least doubled.
- He continues to ride his bike 20 miles daily.
- Decreases health care resource utilization (Wang, J. Bowden, K. 2013)
- Patients want to feel better and be more functional and are satisfied with MILD results
- MILD is relatively low risk
- Anteriolisthesis can decrease interlaminar space but the procedure can still be planned for and carried out
Literature reviewed:
Basu S. MILD Procedure Single Site IRB Study. Clin J Pain 2012; 12: 254-258.
Brown LL. Double blinded, randomized prospective study of epidural steroid injection vs. the mild procedure in patients with symptomatic Lumbar Spinal Stenosis. Pain Practice 2012; 12(5): 333-341.
Chan H, Kelling J. MILD Procedure for lumbar decompression. Pain Practice 2013; 13(2): 146-153.
Deer TR, Kim CK, et al Study of percutaneous lumbar decompression and treatment algorithm for patients suffering from neurogenic claudication. Pain Physician 2012; 15: 451-460.
Durkin B, Romeiser J et al. Report from a quality assurance program on patients undergoing the MILd procedure. Pain Medicine 2013; March 14.
Lingreen R, Grider JS. Retrospective review of patient self –reported improvement and post procedure findings for mild. Pain Physician 2010; 13: 555-560.
Mekhail N, Costandi S et al. Functional and patient-reported outcomes in symptomatic lumbar spinal stenosis following percutaneous decompression. Pain Practice 2012; 12(6): 417-425.
Mekhail N, Vallejo R et al. Long term results of percutaneous lumbar decompression mild for spinal stenosis. Pain Practice 2012; 12(3): 184-193.
Racz G, Heavner J et al. The MILD Procedure. Pain Practice 2013; March 20.
Wang JJ, Bowden K et al. Decrease in health care resource utilization with MILD. Pain Medicine 2013 Apr 11.
Wong WHM. mild Interlaminar decompression for the treatment of lumbar spinal stenosis. Procedure Description and Case Series with 1-year follow-up. Clin J Pain 2012; 28(6): 534-538.